Medication Reconciliation at Discharge
Goal of Medication Reconciliation at Discharge
The goal of medication reconciliation at discharge is to reconcile the medications the patient was taking prior to admission (BPMH) and those initiated in hospital, with the medications they should be taking post-discharge to ensure all changes are intentional and that discrepancies are resolved prior to discharge. This should result in avoidance of therapeutic duplications, omissions, unnecessary medications and confusion.
Discharge medication reconciliation clarifies the medications the patient should be taking post-discharge by reviewing:
- medications the patient was taking prior to admission (BPMH)
- current medications (previous 24-hour MAR)
- new post-discharge medications
Process for Medication Reconciliation at Discharge
An interprofessional, systematic, integrated strategy will reduce medication discrepancies at hospital discharge. This strategy should include tools to support healthcare providers and the patient with discharge reconciliation and should integrate and clarify medication information from all sources. The result should be clear and comprehensive information for the patient and other care providers about post-discharge medications.
The Best Possible Medication Discharge Plan (BPMDP) is the most appropriate and accurate list of medications the patient should be taking after discharge.
Using the Best Possible Medication History (BPMH) and the previous 24-hour medication administration record (MAR) as references, create the BPMDP by evaluating and accounting for:
- New medications started in hospital
- Discontinued medications (from BPMH)
- Adjusted medications (from BPMH)
- Unchanged medications that are to be continued (from BPMH)
- Medications held in hospital *
- Non-formulary/formulary adjustments made in hospital
- New medications started upon discharge
- Additional comments as appropriate (e.g., status of herbal medications/supplements or medications to be taken at the patient’s discretion)
* Medications may be "held" (i.e., stopped temporarily) at the time of admission for a variety of reasons. For example:
- The patient may be at increased risk of a side effect/toxicity (e.g., post-operative bleeding in a patient who takes warfarin regularly)
- The medication may be suspected of causing toxicity and/or lacking efficacy (e.g., blood pressure, pain, diabetes not controlled)
- The medication may not be available on the hospital Formulary and can be substituted with an alternative or temporarily stopped with no clinical risk (e.g., vitamins and other nutritional supplements)
The BPMDP should be communicated to the:
- patient
- community prescriber/family physician
- community pharmacy
- other healthcare facility or service (e.g., long-term care or complex continuing care institution)
Clear patient communication is essential. Each time a patient moves from one healthcare facility to another or to home, providers should review with the patient and/or responsible family member the previous medication regimen alongside the list of medication prescribed at discharge and reconcile the differences. This process should take place both prior to leaving the hospital and again promptly after transition to the new setting of care.
Medication Reconciliation at Discharge Model
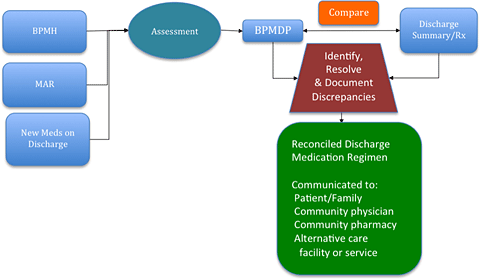
BPMTL: Best Possible Medication Transfer List
An integrated medication reconciliation program has been developed at the University Hospital Network (UHN) in Toronto. Sample discharge medication reconciliation forms from UHN are shown in Appendices 6, 7, and 8.
Team Exercise
This excercise is also available as a PDF.
Discuss the purpose and content of the BPMDP with other members of your team. Is it feasible to provide a BPMDP to patients on your unit? Can you map a process to do this? What barriers are there? How can you overcome these barriers?
Summary
- When preparing a BPMDP, use the BPMH and 24-hour prior MAR
- Ensure changes to medications are documented and communicated to the patient and other healthcare providers

